 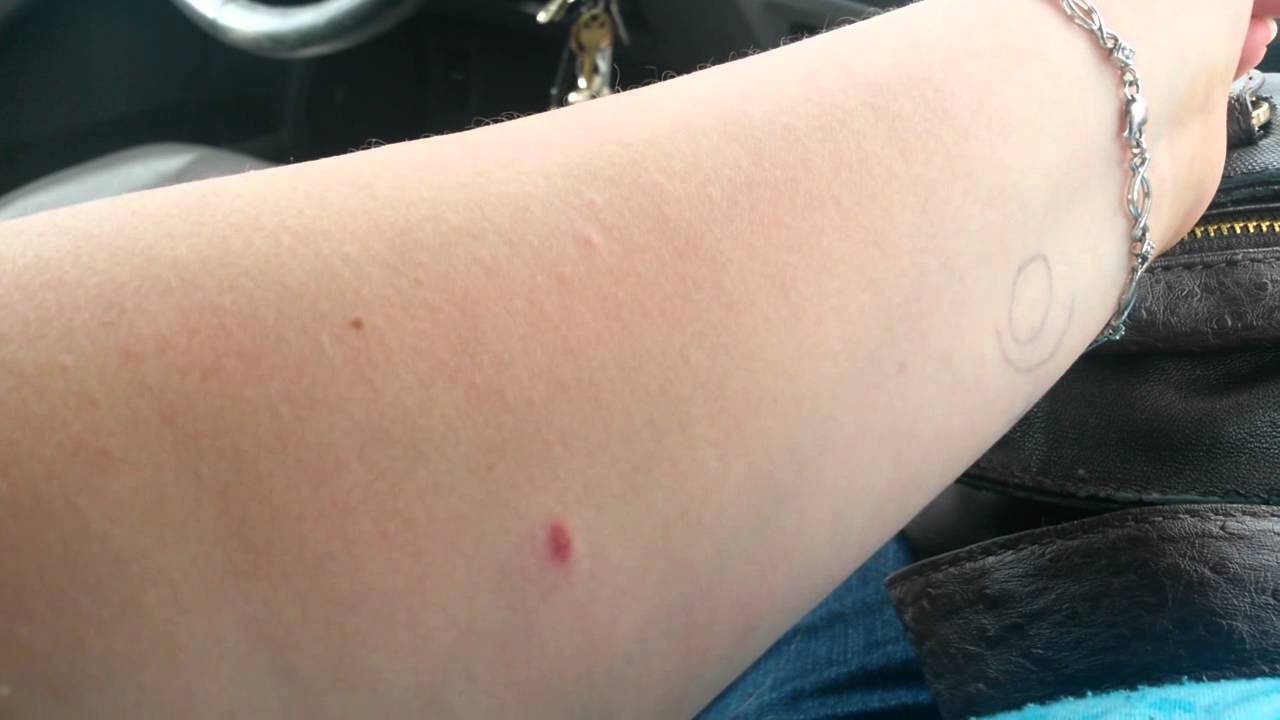
A 10 mm induration may also be considered positive in children under age 4 or people who use injected drugs.Īn induration of 15 mm or more is considered positive in anyone, even people who don’t think they’ve been exposed to TB. The same is true if you live in a high risk environment such as a nursing home, or work in a high risk setting such as a hospital or medical laboratory. have had recent contact with a person with TBĪ doctor may interpret a 5 mm induration as a positive result if you are taking immunosuppressant medications or previously had TB.Īn induration of at least 10 mm may be considered a positive result if you recently immigrated from a country with a high prevalence of TB.If the induration is at least 5 mm, it is considered positive in people who: If you have symptoms or know you’ve been exposed to someone with TB, a doctor may recommend you get another test. work in a hospital, medical laboratory, or other high risk settingĪn induration of less than 5 millimeters (mm) is a negative result.recently immigrated from a country with a high incidence of TB.are taking immunosuppressant medication.have had recent contact with someone with TB.The results of these tests can determine if you should receive treatment and with what type of medication. If your skin test is positive or if you may have a false negative, a doctor may administer a blood TB test. This may occur years after the initial infection.Ī doctor may treat active TB with a combination of medications for about 6 months.Ī blood or skin test can help healthcare professionals diagnose TB. According to the Centers for Disease Control and Prevention (CDC), 1 in 10 people with a latent TB infection will develop an active reinfection. If this happens, you may experience symptoms such as:ĭoctors may treat latent TB to prevent future active disease. Latent infection can eventually reactivate as a secondary TB infection. Latent TB means you have an infection but no signs or symptoms. It is caused by an infection of bacteria called Mycobacterium tuberculosis ( Mtb).Įxposure to Mtb can result in either active TB disease or a latent TB infection. If you continue to have this issue please contact to HealioĪ 13-year-old previously healthy female is seen by her primary for evaluation of some unexplained painful bruising of her upper extremities that began about 2 weeks earlier.TB is a highly contagious disease that primarily affects your lungs and respiratory system. She denied any injury or recent illness, and she was taking no medications. The problem began as erythematous bumps that were somewhat painful and appeared to be progressive with more areas of spontaneous, firm swelling over the first week, followed by bruising. The bruises seem to be appearing almost exclusively on the extensor surfaces of her arms, but she also complains of some pain on her lateral, lower left leg, but no skin changes were noticed, and she has had no fever recently or any other systemic symptoms. 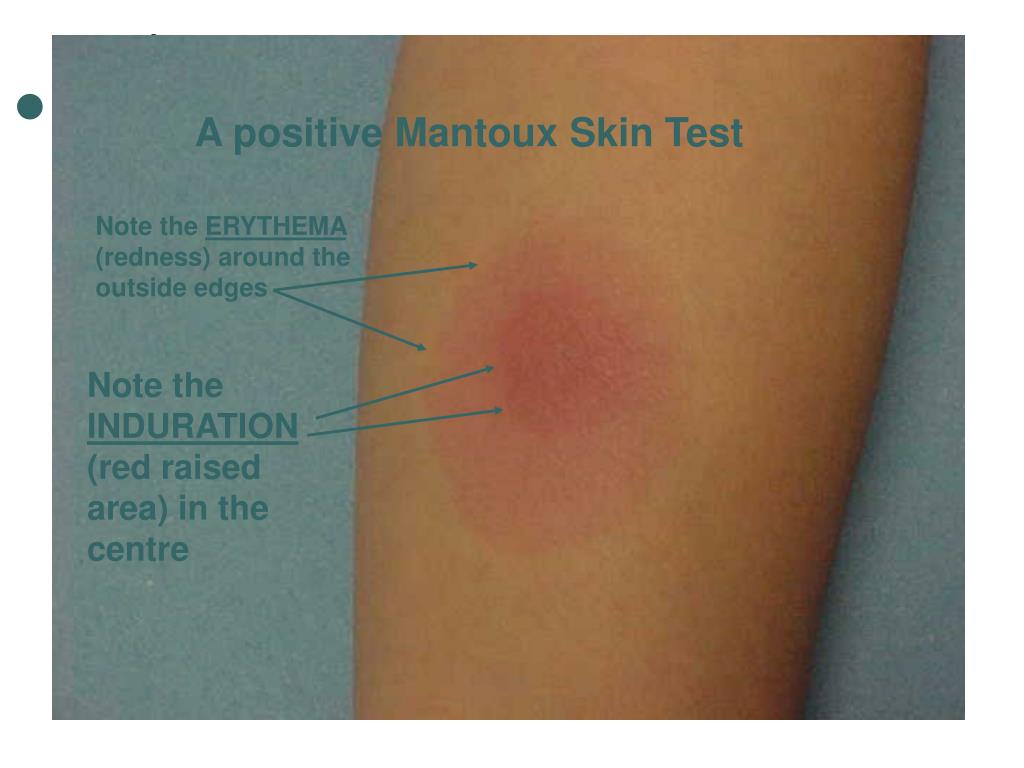
On examination, her vital signs are normal, and her skin exam reveals the apparent bruising described above ( Figures 1-4), with some underlying swelling. The patient also has an impetiginous lesion near her chin ( Figure 5), which further history revealed that she has had a sore in that location before, but cannot remember when. 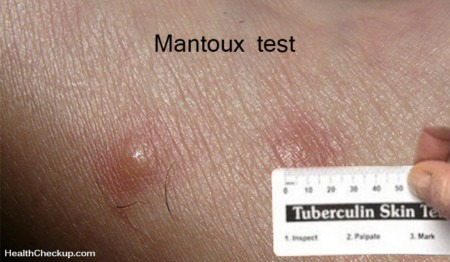
Otherwise, her skin is clear, with no petechiae, other areas of bruising or other lesions seen, and the rest of her exam is normal. The lesion on her chin turned out to be cutaneous herpes simplex infection, an uncommon trigger for erythema nodosum (B), which is thought to be a delayed hypersensitivity reaction resulting in a panniculitis with a surrounding inflammatory reaction. It usually occurs on the anterior aspects of the lower legs (shins), but can occur anywhere. It is most commonly associated with group A streptococcal infections, but can be triggered by a wide variety of infectious and noninfectious causes. It is a clinical diagnosis with a good history and physical exam, which often reveals the history of painful bumps with varying degrees of erythema that usually goes through some color changes, similar to a bruise within a couple of weeks.Ī biopsy revealing inflammation about the subcutaneous fat without vasculitis would help confirm the diagnosis, but is usually not necessary if the clinical course is typical and no menacing underlying disease is suspected. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
